
La piattaforma di decisioning e automazione dei flussi di lavoro basata su IA
Genera risultati trasformativi per la tua impresa

How are you looking to make an impact?
Pega is architected differently to run your most critical journeys.
Commonwealth Bank of Australia supera le aspettative dei clienti grazie a conversazioni personalizzate
La banca utilizza Pega Customer Decision Hub per suggerire e personalizzare in modo intelligente la next best action per ogni cliente.
“Pega e il suo motore di Customer Engagement sono stati un enorme passo avanti per noi. Ci permette di orchestrare tutti i nostri canali.”

Consigliato per te
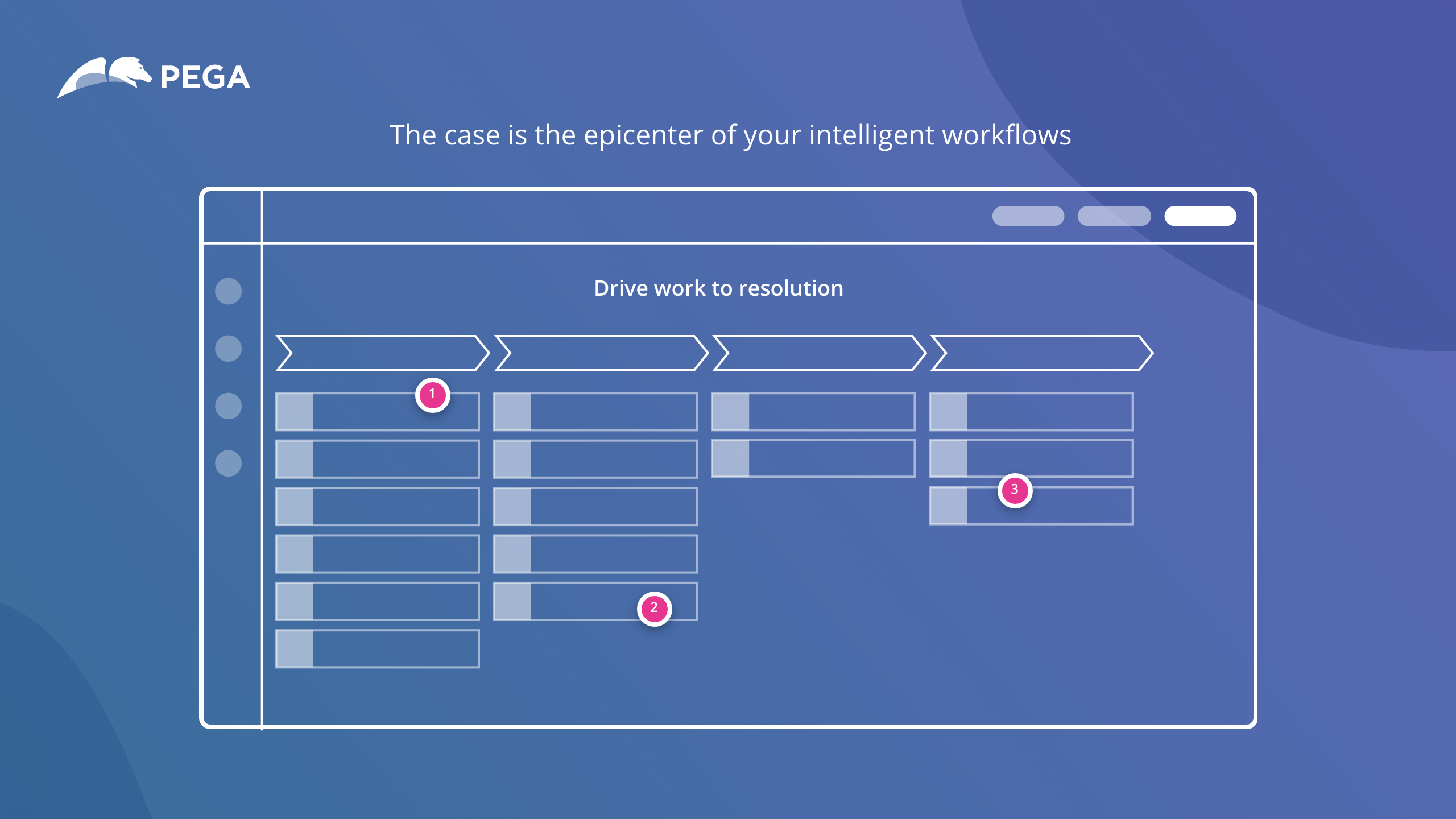
Demo interattiva
Fai il tour di Pega Platform
Fai il tour.
Demo interattiva
Crea un'app di livello enterprise in pochi minuti
Prova Pega GenAI.

Evento in presenza
PegaWorld iNspire 2024
Le registrazioni al PegaWorld iNspire sono aperte! Il nostro evento di punta offrirà tante occasioni per trovare l’ispirazione, usare l’immaginazione e fare networking.

40 anni di innovazione
software sono solo l'inizio
software sono solo l'inizio
Inizia con noi il tuo percorso verso un'azienda autonoma in fatto di operazioni e ottimizzazione.









